Spasticity Management Clinic
Gillian Harte

Gillian is a Clinical Specialist Physiotherapist working within the Stroke Service at Tallaght University Hospital. She holds a BSc in Physiotherapy from the Royal College of Surgeons in Ireland (RCSI) and an MSc in Neurological Rehabilitation from the University of Plymouth, and works primarily in stroke rehabilitation.
Introduction:
Spasticity is a condition of disordered muscle function as a result of an upper motor neuron lesion. Untreated it can lead to a host of complications such as pressure ulcers, contractures, pain and progressive decline in functional ability. Clinical Practical guidelines recommend that this condition should be appropriately managed within a specialised service to prevent complications.
Methodology:
There was no dedicated spasticity management clinic in TUH departments despite large stroke and neurology departments. This placed patients at risk of complications with increased risk of hospitalisation and A&E presentation, and limited the effectiveness of therapy, prolonging hospital stay. The Meath Foundation provided a grant to employ a part- time clinical specialist physiotherapist for six months.
Referrals were accepted for patients under the care of a Tallaght University Hospital Consultant or within the catchment area. Initial assessments included assessment of spasticity and functional implications. Treatment pathways were agreed and a procedure developed.
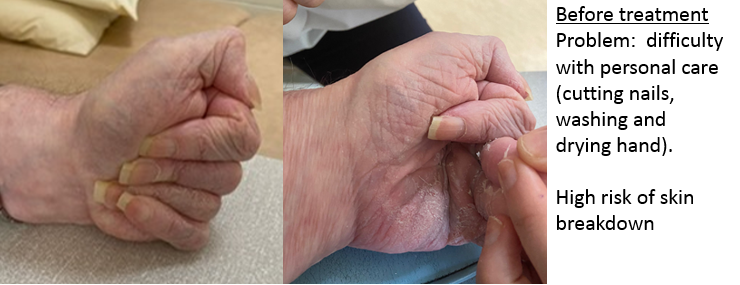
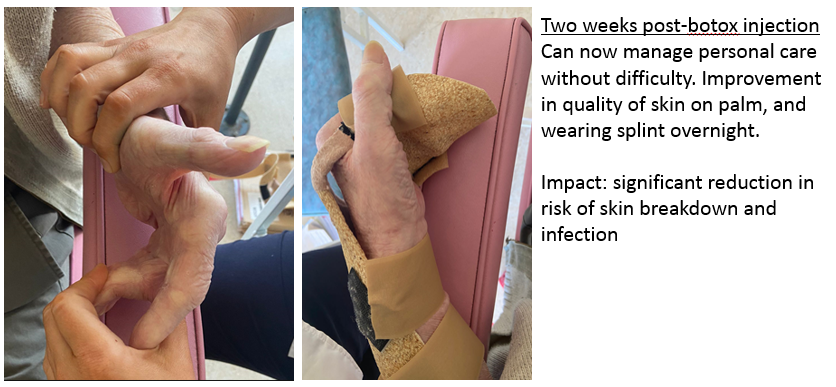
Patient Goals
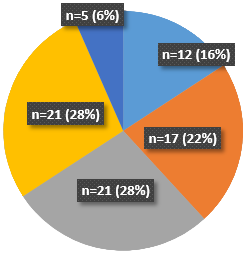
- 28% of patients wanted to improve their mobility.
- 28% to improve passive function.
- 22% to reduce involuntary movement.
- 12% to reduce their pain.
- 6% to regain active arm function.
Clinical Interventions
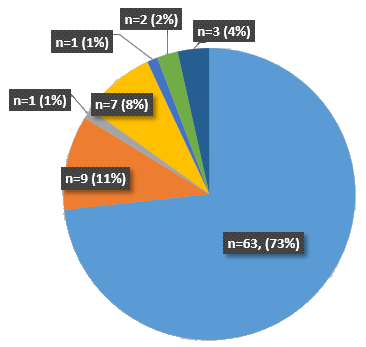
- 73% of Patients were given Botox.
- 11% given specific advice to patient and treating physiotherapist.
- 8% of Patients were given an exercise programme.
- 1% had advice sent to their GP.
- 1% were referred to a TUH Consultant.
Outcomes after Botox
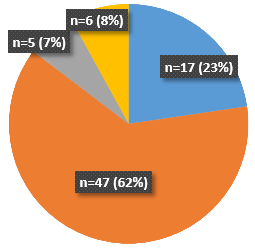
- 62% of patients reported that their goal was achieved.
- 23% reported that their goal was exceeded.
- 8% reported that their goal was not achieved.
- 7% reported that their goal was partially achieved.
Did the Patients feel listened to by staff?
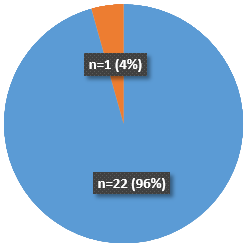
- 96% said ‘Yes, definitely’.
- 4% said, ‘Yes, somewhat’.
Patients were asked if they felt there was a clear plan for their care after visiting the clinic?
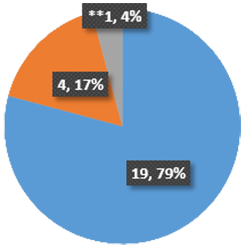
- 79% said, ‘Yes, definitely’.
- 17% said, ‘Yes, somewhat’.
- 4% said, ‘No’.